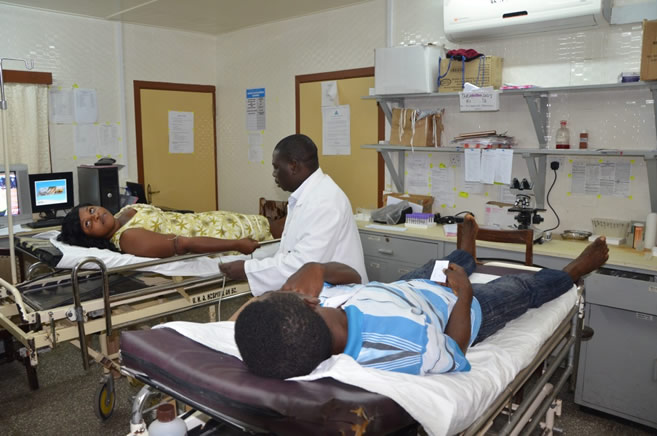
We are currently facing a primary healthcare crisis in Nigeria and speedy intervention is needed to enhance access to health care for our ever growing population.
The latest data from the World Health Organization (WHO) reveals that Nigeria’s physician-to-patient ratio is 4 doctors per 10,000 patients and patients often wait hours to be seen. In the US the ratio is 26 doctors per 10,000 people and 28 in the UK.
Nigeria repeatedly falls short on its 2001 commitment to spend at least 15% of its budget on health. Last year just 3.9% was allocated.
Register for Tekedia Mini-MBA edition 20 (June 8 – Sept 5, 2026).
Register for Tekedia AI in Business Masterclass.
Join Tekedia Capital Syndicate and co-invest in great global startups.
Register for Tekedia AI Lab.
The Nigerian Medical Association (NMA) advised there are only 40,000 doctors in an estimated population of 196 million.
A WHO report by Uta Lehmann and David Sanders from the School of Public Health University of the Western Cape, says:
‘The use of community health workers has been identified as one strategy to address the growing shortage of health workers, particularly in low-income countries. Using community members to render certain basic health services to the communities they come from is a concept that has been around for at least 50 years. There have been innumerable experiences throughout the world with programmes ranging from largescale, national programmes to small-scale, community-based initiatives’ (Evidence and Information for Policy, Department of Human Resources for Health Geneva, January 2007)
Community health workers have the potential to enhance primary care access and quality, but remain underutilised in Nigeria.
It is common knowledge that we do not have trained physician associates or assistants in primary care facilities to support medical doctors in providing primary care services; rather what we have in some communities are quacks, people parading themselves as medical doctors with no medical qualification whatsoever.
But I don’t see any reason why we should not welcome the idea of training physician associates or assistants to fill in the gap for medical staff shortage, when other developing and developed countries that have better healthcare systems do have them.
In Nigeria we do not have enough doctors per population or geographical area, This is the time to train more community health care workers as this would help in the much needed awareness creation and community based interventions for managing long term conditions, reducing childhood illnesses due to lack of immunisation. Trained birth attendants will also help reduce maternal mortality and community nursing care will reduce infant mortality.
In a typical medical centre in the UK for instance, healthcare assistants, advanced nurse practitioners, health trainers, clinical pharmacists or prescribers, work alongside doctors to provide patient centered care. This helps to reduce the work load on the doctors as these other clinicians and allied health workers have enough training and experience to manage long term conditions and participate in triage system.
In the UK, a lot of research has been done and there are calls to increase the health work force in the National Health Service (NHS) through the utilisation of community-based lay workers.
In Brazil, community health workers receive basic training in disease identification and monitoring, immunisation, screening and health promotion. They support patients with medication adherence and chronic disease monitoring and liaise proactively with doctors and practice nurses.
Community healthcare workforce could be utilised effectively in emergency care or first aid. In most public and private settings in Nigeria, there are no ambulance or paramedic services; having well trained community first aid responders would go a long way to save lives in times of emergency for example; cardiac arrest, collapse, and respiratory distress. Having a health unit manned by well-trained first aid responders in all public places like markets, motor parks etc is highly essential.
Healthcare provision anywhere in the world is capital intensive but we can start from the basics; we can reduce the burden or costs in secondary healthcare provision especially in our public hospitals if we lay more emphasis on health promotion, patient health education and encourage people to engage in healthy living and self-care.
Another important way we could ensure we have enough medical/healthcare practitioners to address the primary healthcare needs in Nigeria is to reduce the constant brain drain by retaining our health professionals post graduation.
The Federal Government invests a lot of funds in Government owned Universities to train medical/healthcare professionals, only for them to migrate after graduation to practice in other countries. If we are going to invest funds in medical/healthcare education for our doctors, pharmacists, nurses, optometrists etc we should create jobs as well so the Nigerian populace could benefit from their expertise.
Integrated healthcare practice at all levels is an efficient way of providing patient centered care where every member of the healthcare team contributes their own quota. Community healthcare workers are well placed to offer advice on healthy living and self-care in the language people of a specific demographic area would understand. Hypertension, Chronic Kidney Disease, Type 2 diabetes mellitus, malaria, HIV/AIDs are among the diseases that could be prevented or well managed through patient education and lifestyle modification.
The role of health education cannot be overemphasized. For instance, there is still some form of stigma around epilepsy in some areas in the country; where people who are epileptic are believed to be possessed by some sort of evil spirits, in an unfortunate event of epileptic fits in public places, patients are not well cared for and objects like spoon etc. are inserted into their mouths in the believe that it keeps the airways open, this could be a choking hazard and has made recovery time worse for some patient. Community healthcare workers could perfectly fill that gap of providing basic health education and public health enlightenment.
Addressing the primary healthcare crises in Nigeria is no mean feat, but we need to look at the issue holistically, it involves a multifaceted, public/private partnership, but the Government has to lead on this through enacting relevant laws and provision of training programs, monitoring and evaluation etc.
I strongly believe a systematic integration of community health workers at scale could be an effective and a rapidly implementable approach to the current primary care workload crisis in Nigeria.
‘Without health, life is not life; it is only a state of languor and suffering’.
Francois Rabelais



